Artificial Disc Replacement
This month I have chosen a topic that seems like the perfect solution to a significant problem---Artificial Disc Replacement surgery. Recently, I have had more questions posed to me on this matter. As I’m not a neurosurgeon, I don’t have all the answers, but wanted to obtain more edification on the subject.
Artificial Disc replacement (ADR) or Total Disc Replacement is a surgical procedure that replaces a worn/degenerated disk in the neck or lower back with a medical-grade metal or a combination of medical-grade metal and medical-grade plastic prosthetic device. This surgery is done in lieu of a fusion with the thought that it better preserves the motion of the spine, thereby closer mimicking your overall norm. Fusions by their nature will cause some form of motion limitation/loss. When you start limiting the range of motion (ROM) you change the person’s posture/stature and how their body responds to the loads and forces placed on the spine throughout normal daily activities of life to increased stresses with hobbies and physical activities.
Artificial disk replacement is not appropriate or rather not a viable option for all patients with spinal pain. As with any surgery, there are several variables that need to be weighed and factored. In general, good candidates for disc replacement have the following characteristics3:
- Spinal pain caused by one or two problematic intervertebral discs---while multilevel procedures are now approved, too much pathology or degeneration will place the patient in a category where a fusion is a better solution.
- No significant facet joint disease or bony compression on spinal nerves. Again if there is too much going on a disc replacement is not likely to make a significant difference, so why do the surgery in the first place.
- Body size that is not excessively overweight---if a person’s body habitus is significantly obese, the surgery will not provide a significant long-term benefit. This is a surgery better catered to those who desire to remain more active.
- No prior major surgery on the lumbar spine
- No deformity of the spine (scoliosis)
Artificial disc implants are designed to be placed into the disc space from the front and center position. To get there, the surgical approach is performed anteriorly (from the front)---while this is relatively routine in the neck, it is quite a bit more complicated in the lower back, reaching the spine and disc working around the abdominal contents (retroperitoneal) from an incision at or near the front of the abdomen. Working behind the abdominal contents, the spine is reached by moving the major blood vessels that bring blood to and from the legs off to the side. These vessels are normally found directly on the front surface of the spine, and must be moved and protected in order to work safely on the spine. Because of these needs, a vascular or general surgeon commonly acts as co-surgeon with the spine surgeon during anterior spinal procedures such as total disc replacement1.
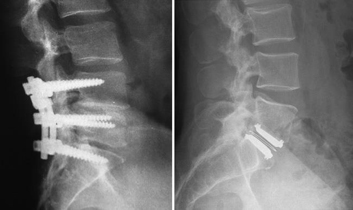
Below you will see a radiograph of a Lumbar (lower back fusion) vs a ADR---this will give you some comparison as to the dynamics of each surgery3.
Isador Lieberman, MD, MBA, FRCS(C) an Orthopaedic and Spinal Surgeon from The Cleveland Clinic Foundation in Cleveland, OH had this testimonial2:
- Disc replacement represents another spectrum of treatment for patients suffering from degenerative discs.
- The indications for disc replacement are limited - this will not be the absolute cure for all that ails the spine.
- Surgeons who perform this surgery must be trained and should have past experience with anterior spine surgery.
- The risks include misplacement, dislodgement, injury to surrounding organs and vessels during implantation, as well as all of the usual risks of spinal surgery.
- The longevity of artificial discs is yet known (approval for the process was granted 2004). If it only lasts 10 years, the patient will definitely need further surgery.
- Revision disc replacement surgery will be a life-threatening operation.
- Patients need to remember that back pain is not life threatening, but spinal surgery can be.
Below is the conclusion of a study, found on the NCBI website:
Lumbar fusion has been developed for several decades and became the standard surgical treatment for symptomatic lumbar degenerative disc disease (DDD). Artificial total disc replacement (TDR), as an alternative for spinal arthrodesis, is becoming more commonly employed treating lumbar DDD. It is still uncertain whether TDR is more effective and safer than lumbar fusion. To systematically compare the effectiveness and safety of TDR to that of the fusion for the treatment of lumbar DDD, we performed a meta-analysis. Cochrane review methods were used to analyze all relevant randomized controlled trials published up to July 2009. Five relevant randomized controlled trials involving 837 patients were identified. Patients in TDR group have sightly better functioning and less back or leg pain without clinical significance, and significantly higher satisfaction status in TDR group compared with lumbar fusion group at the 2-year follow-up. But these outcomes are highly influenced by the study with BAK cage interbody fusion, the function/pain and patient satisfaction status are no longer significantly different between two groups after excluding this study. At 5 years, these outcomes are not significantly different between comparing groups. The complication and reoperation rate of two groups are similar both at 2 and at 5 years. In conclusion, TDR does not show significant superiority for the treatment of lumbar DDD compared with fusion. The benefits of motion preservation and the long-term complications are still unable to be concluded. More high-quality RCTs with long-term follow-up are needed4.
While researching this topic, a lot of the articles appeared to be dated, while the bulk of information is certainly representative of the surgery---medicine is a fluid science, what is true today may be altered tomorrow.�Therefore, I reached out to some of my neurosurgeon contacts---to get the more up to date, cutting edge answers and this is what they said:
- ADR can be a very useful procedure, but it is dependent on patient selection---meaning, unless the patient fits into the appropriate parameters it is better to do the fusion.
- The appropriate parameters are very small niche---this is not a procedure that will fit a large percentage of the population
- ADR is much better suited to the neck region---there is some question if performing in the lower back is a reasonable consideration
- Quality of the surgeon is very important, both in their evaluation of the candidate population and skill in the OR.
My overall evaluation on the matter is that ADR can be a successful modality of treatment for problem discs provided you fit inside the box.�However, in saying this, there are numerous risks and an uncertain outcome---as with any surgery, you really don’t know what you got until it’s completed.�My recommendation would be to take care of/protect what you got today, by practicing good body mechanics, posture and developing a good home exercise program with a qualified Physical Therapist.�If you are past this point, then consider less invasive options first, such as regenerative injections which aim to help your body repair itself, thereby staving off a surgical procedure.
References:
- https://www.spine-health.com/treatment/back-surgery/artificial-disc-replacement-or-spinal-fusion-which-better-you
- https://www.spineuniverse.com/treatments/emerging/artificial-discs/spine-surgeons-speak-out-about-artificial-disc-replacement
- https://orthoinfo.aaos.org/en/treatment/artificial-disk-replacement-in-the-lumbar-spine/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2989192/
- https://www.hopkinsmedicine.org/healthlibrary/test_procedures/neurological/lumbar_disk_replacement_135,1
